Angioplasty, Atherectomy and Stenting
 Arteries, blood vessels that carry oxygen-rich blood to all the parts of the body, are normally flexible and smooth on the inner side, but deposits of cholesterol, calcium, and fibrous tissue (plaque) can build up on the inner walls of the arteries, making them hard, stiff and narrow. This process of thickening and hardening of the arteries is called atherosclerosis. Atherosclerosis can reduce or completely stop the flow of blood through them, causing damage and pain to the part of the body that the arteries supply.
Arteries, blood vessels that carry oxygen-rich blood to all the parts of the body, are normally flexible and smooth on the inner side, but deposits of cholesterol, calcium, and fibrous tissue (plaque) can build up on the inner walls of the arteries, making them hard, stiff and narrow. This process of thickening and hardening of the arteries is called atherosclerosis. Atherosclerosis can reduce or completely stop the flow of blood through them, causing damage and pain to the part of the body that the arteries supply.
Angioplasty is the surgical procedure that is performed to widen these blocked or narrowed arteries. During angioplasty, your surgeon inflates a small balloon within the narrowed artery to widen and improve the blood flow. Often, your surgeon may insert a stent, a tiny meshed tube to support the artery wall and keep the artery wide open
Procedure
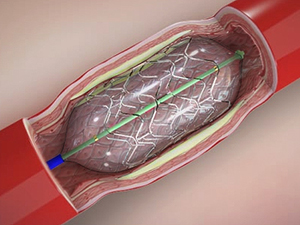
Angioplasty is performed under local anaesthesia. A dye is injected into the body to view the blood flow through the arteries, and X-rays are taken. Using these X-ray images, your surgeon inserts a thin guide wire through a blood vessel in the groin area and extends it up to the blocked artery. A balloon catheter (thin tube) is then threaded through the guide wire to the narrowed artery. The balloon catheter has a deflated balloon at its tip, which is inflated at the site of blockage. The balloon widens the artery by compressing the plaque against the wall of the artery. Your surgeon may also insert a wire mesh tube called a stent along with the balloon catheter to help keep the artery open and prevent it from narrowing again. The balloon and the catheters are removed, while the stent is left in place to keep the artery wide open and allow free flow of blood.
Post-procedure care
Following the surgery, you will be able to go home the same day or may have to remain in the hospital for not more than 2 days. You will be able to start walking in 6 to 8 hours after the procedure.
Risks & Complications
Risks and complications following this procedure are rare. However, some specific complications for angioplasty are
- bleeding from the catheter insertion site
- irregular heartbeat
- chest pain during procedure
- blood vessel damage from the catheter
- kidney damage from dye used with angiogram
- re-stenosis (re-accumulation of plaque or scar tissue causing narrowing or blockage of the coronary artery; occurs within 6 months)
- blood clots
- dislocation of stent
Atherectomy
Arteries, blood vessels that carry oxygen-rich blood to all the parts of the body, are normally flexible and smooth on the inner side. However, plaque (deposits of cholesterol, calcium, and fibrous tissue) can build up on the inner walls of the arteries. These plaques can make the arteries hard, stiff and narrow, reducing or completely blocking the flow of blood through them. Plaque can be removed by a procedure called atherectomy.
Indications for Atherectomy
Atherectomy is indicated for narrowed arteries that cannot be treated with
- Angioplasty and stenting: procedure where a thin tube with a balloon and/or small mesh tube is inserted through a large artery in the leg to widen the blockage
- Bypass surgery: blood vessel re-directed to avoid arterial blockage
Atherectomy is sometimes used as a complement to angioplasty and stenting where hardened plaques are first removed to an extent to allow the insertion of the balloon and stent, which then widen the artery.
Procedure
Atherectomy is performed under local anesthesia. A thin guide wire is threaded into the blocked artery with the help of a small needle that is inserted into a blood vessel in the groin area. This guides a catheter or a thin tube to the blockage, through which a dye is injected into the artery, and X-rays are taken to view the path of the artery.
Your surgeon then inserts an atherectomy catheter attached with a blade, grinding bit, or laser filament at its tip through the guide wire to the narrowed part of the artery which is used to scrape away the plaque. Your surgeon may pass the catheter several times to cut away major parts of the hardened plaque. A collecting chamber or suction system at the tip of the catheter removes the plaque particles while it is being scraped off. Once the hardened plaque is removed, your surgeon inserts a stent, a tiny mesh tube, to support and keep the artery wall wide open, preventing it from narrowing again. Once the treatment is complete, the catheter is removed.
Post-operative Care
Following the procedure, you are advised to lie flat for some time. If bleeding occurs from the insertion site, you need to have pressure applied to stop the bleeding. You need to inform the nurse if you develop swelling, pain or bruising at the site of the catheter insertion. You will be asked to drink a lot of fluids to eliminate the dye injected into your body. Following the surgery, you will be able to go home the day after the atherectomy and you can return to your normal activities in a day or two, but you should refrain from engaging in certain strenuous activities.
Risks & Complications
The possible risks and complications of an atherectomy may include:
- Bleeding at the site of insertion
- Infections
- Re-blockage of the artery by plaque formation
- Heart attack due to closure of the artery, which requires emergency bypass surgery
- Damage or injury to the artery leading to loss of blood
- Clot formation in the leg or arm, which can lead to embolism (pieces of blood clot can break off and travel to the lungs or brain causing chest pain or stroke, respectively)







