Carotid Artery Disease
What is Carotid Artery Disease?
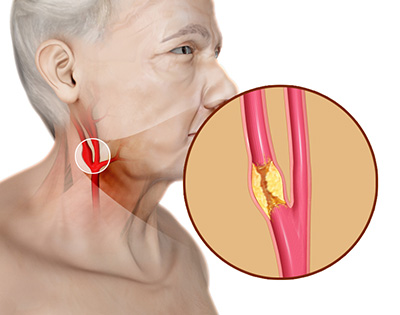
Carotid Artery Disease (CAD) is a condition where the carotid arteries become narrowed or blocked (‘occluded’) by a buildup of plaque that is made up of fatty deposits called atherosclerosis.
You have two main carotid arteries that run up the neck and then split into internal and external carotid arteries. The internal carotid arteries supply oxygen-rich blood to your brain. The external carotid arteries supply oxygen-rich blood to your face, scalp, and neck.
Carotid Artery Disease is the result of the main carotid arteries becoming partially or fully blocked with this waxy plaque, preventing adequate blood flow to the brain.
This plaque can cause:
- Stroke - a severe medical emergency
- Trans-ischaemic attack (TIA) colloquially known as a ‘mini stroke’, and
- Amaurosis fugax (a painless temporary loss of vision in one or both eyes)
What causes Carotid Artery Disease?
Lifestyle conditions are mostly to blame for the damage caused to the arteries.
Major factors that contribute to this damage include:
- Smoking
- A history of smoking
- High levels of certain fats and cholesterol in the blood (hypercholesterolaemia)
- High blood pressure
- High levels of sugar in the blood due to insulin resistance or diabetes
When these factors cause damage, your body starts a healing process. The healing may cause the walls of the arteries to become less smooth, making them more likely to catch the fatty plaque as it passes through in the blood.
Blood clots from this attempt at healing can also create a perfect catchment area for the plaque to congregate. The buildup can subsequently cause carotid artery disease, and potentially result in a stroke.
What are the signs/symptoms of Carotid Artery Disease?
Carotid artery disease can go undetected (or be asymptomatic) until a problem develops like:
- Stroke
- Mini-stroke
- Visual disturbances (amaurosis fugax)
- Visual aura
- Temporary blindness (usually in one eye)
- One sided weaknesses
- Collapse/fainting
- Dizziness
- Tinnitus/ringing in the ears
How will Carotid Artery Disease affect my health?
Carotid Artery Disease that is under surveillance should be monitored closely with ultrasound and reviewed by your doctor. You will probably be placed on a blood thinner as well.
Untreated CAD can be responsible for catastrophic life-altering and life-threatening stroke. Symptoms of stroke are severe, and can include half or full body paralysis.
What are the stages of Carotid Artery Disease?
Carotid Artery Disease can be long in the making, and asymptomatic for a very long time. The stages can ‘fast-forward’ to a stroke or other life-altering event seemingly instantly if lifestyle improvements, such as monitoring of blood sugar, cholesterol and pressure, are not prioritised on a regular basis.
Once detected, CAD should be monitored on a regular basis by ultrasound and under the guidance of a Vascular Surgeon. This way, if it progresses to a point where the risk of stroke is greater than the risks associated with surgery, appropriate surgery can be performed in a timely fashion.
I think I have Carotid Artery Disease – What should I do?
Carotid Artery Disease should not be left unassessed or unmonitored. It is best to be proactive in seeking regular checkups with your GP, especially if you are in the risk groups mentioned above, in ‘What causes Carotid Artery Disease’.
Sometimes, if you have other vascular problems, or even heart problems, your doctor will look specifically for Carotid Artery Disease during an examination, because if you have blockages in some arteries you are at increased risk of having blockages in others.
On physical examination, your doctor might routinely listen to your neck with a stethoscope, which will sometimes reveal a “bruit”, which is an unusual noise that can indicate the presence of a blockage in the vessels. This will normally result in you being sent to have an ultrasound called a ‘Carotid Ultrasound’.
What if I don’t have my Carotid Artery Disease treated?
Some people with Carotid Artery Disease do not require intervention because it never progresses to a point where intervention is warranted.
However, everyone with Carotid Artery Disease should be under surveillance to monitor whether the disease is progressing or not, so that treatment can be provided as soon as possible.
The risks of leaving CAD unmonitored or untreated can be life-altering due to stroke, or fatal.
What treatment options does SVS offer for Carotid Artery Disease?
Sydney Vascular Surgery offers a range of treatment options for Carotid Artery Disease, from conservative management, through to surgical treatments.
Conservative management
If your tests and diagnoses suggest that the Carotid Artery Disease is manageable by conservative measures, you will need to simply monitor your symptoms and maintain regular visits with your GP and surgeon.
Also key to your ongoing wellbeing is your action towards improving your fitness and leading a healthy lifestyle, namely by not smoking at all, or quitting smoking. If you would like help to quit smoking, your GP will have many options to provide you with the support you need.
Surgery
Two main surgery methods for treating CAD are:
- Carotid Endarterectomy
- Carotid Stent Surgery
Carotid Endarterectomy
This is an open procedure that involves an admission into hospital the day before the procedure, and a 3-5 day stay in hospital, in ICU, following the procedure.
A Carotid Endarterectomy is performed under a local anaesthetic with sedation and usually takes approximately 2 hours.
It is important that you are awake during the procedure so that the surgeon can talk to you and ensure that you do not have any stroke-like symptoms during the procedure. Fortunately, due to the sedation it is unlikely you will remember anything.
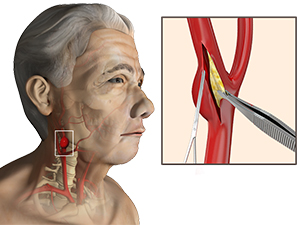
During a Carotid Endarterectomy the surgeon makes a vertical or curved incision in the neck to isolate the affected carotid artery. The aim of this procedure is to clear the buildup from inside the artery, so the surgeon will clamp the artery, make an incision and clean out the waxy residue. The clean artery will then be sutured, sometimes with the addition of a ‘patch’ made from another vein or from a synthetic material, and finally, the neck incision will be closed.
Carotid Stenting
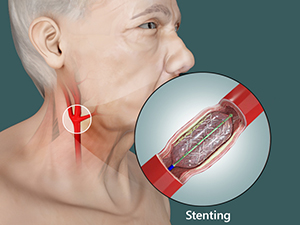
Carotid Stenting is the insertion of a stent (a fine metal cylindrical scaffold) through a small incision in the groin. Special X-ray equipment and dye allow the surgeon to safely move the stent from your groin to your carotid artery in your neck.
The stent is designed to keep the artery open and to trap any plaque.
Stenting is minimally invasive, since the surgeon will only make small incisions in the groin area, rather than a larger neck incision.
The surgeon will consider very carefully whether you have disease morphology that is suitable for stenting. Stenting is usually reserved for patients who cannot undergo a Carotid Endarterectomy.
Stenting is performed under angiographic control, with a local anaesthetic and sedation and usually takes approximately 2 hours. The hospital stay and admission is similar to the Carotid Endarterectomy.
After treatment
Unfortunately, Carotid Artery Disease cannot be cured, but rather, treated with surgery, adjustment of lifestyle factors and the taking of blood thinning medications. Sometimes, even with diligent following of the doctor’s instructions and good management of lifestyle factors, the disease can recur, so it is important to have ongoing surveillance with your doctor.
This will usually involve ultrasound of the carotid arteries, along with consultation. By doing this on a regular basis, you and your doctor can identify if your disease is recurring or progressing and offer adjustments to your treatment. The doctor can can also perform further surgery if neccesary, before you start experiencing debilitating symptoms.
Helpful Links:
Asymptomatic Carotid Disease http://www.anzsvs.org.au/patient-information/asymptomatic-carotid-disease/
Carotid Artery Disease http://www.anzsvs.org.au/patient-information/strokes-tias-and-carotid-surgery/
Carotid Endarterectomy http://www.anzsvs.org.au/patient-information/asymptomatic-carotid-disease/
Carotid Stent http://www.anzsvs.org.au/patient-information/asymptomatic-carotid-disease/







