Varicose Veins
What are Varicose Veins?
Varicose veins, otherwise known as ‘varicosities’, are veins that have become distended and tortuous.
When they are close to the skin’s surface, they are raised, dark and knobbly in appearance. They range in size from very small (2-3mm wide), to very large (2-3cm wide). They represent a spectrum of venous disorders from simple spider veins to varicose veins and advanced skin changes such as ulceration.
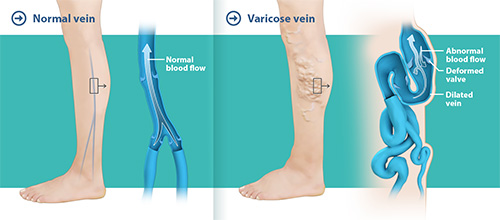
Veins become ‘varicose’ when valves inside the veins stop working as well as they should. These ‘leaflet valves’, when healthy, open and close rhythmically to push blood towards the heart, preventing a backward flow.
When the leaflet valves no longer meet in the middle of the vein properly, blood flows backwards and pools, resulting in increased pressure within the venous system resulting in distended and tortuous veins.
What causes Varicose Veins?
Varicose veins are more common in women than in men, and are linked with heredity.
Other related factors are:
- Pregnancy
- Obesity
- Menopause
- Ageing
- Prolonged standing
- Leg injury
- Abdominal straining, and
- History of deep venous thrombosis
Less common causes of varicose veins are (DVT is one of the main causes of venous hypertension)
- postphlebitic obstruction and/or incontinence - chronic complications after DVT), or
- venous and arteriovenous malformations - abnormal formation or ‘tangle’ of veins and arteries in the body).
Varicose veins can affect any vein in the body, but most commonly affect the legs because legs are subject to high pressure when standing. They can also extend up into the groin and genital area.
They can be worse after strenuous exercise, long periods of standing, after air travel and during and after pregnancy. It is not uncommon for varicose veins to re-occur, even after treatment.
What are the signs/symptoms of Varicose Veins?
The signs and symptoms of varicose veins include:
- Aching,heavy legs (often worse at night and after exercise).
- Appearance of spider veins (telangiectasia) in the affected leg.
- Ankle swelling.
- A brownish-blue shiny skin discoloration near the affected veins.
- Redness, dryness, and itchiness of areas of skin, known as stasis dermatitis or venous eczema, because of waste products building up in the leg.
- Cramping, especially when making a sudden move, such as standing up.
- Minor injuries to the area may bleed more than normal and/or take a long time to heal.
- In some people the skin above the ankle may shrink (lipodermatosclerosis) because the fat underneath the skin becomes hard.
- Restless legs syndrome appears to be a common overlapping clinical syndrome in patients with varicose veins and other chronic venous insufficiency.
- Whitened, irregular scar-like patches can appear at the ankles. This is known as atrophie blanche or Livedoid vasculitis
How will Varicose Veins affect my health?
Varicose veins can be unsightly, but they can also affect your health by causing:
- Pain and ache in the legs
- Swelling in the legs
- Irritating skin conditions around the vein
They may also be a factor in the development of more serious conditions such as:
- Cellulitis - bacterial infection of the skin
- Superficial venous thrombosis (SVT) - a blood clot near the surface of the skin
- Deep vein thrombosis (DVT) - a potentially fatal blood clot
- Non-healing wounds, such as skin ulceration.
What are the stages of Varicose Veins?
The clinical stages of increased venous pressures evolve from no symptoms to spider veins to varicose veins to leg swelling. Further progression leads to clinically significant changes such as pigmentation to eczema and finally to ulceration. The progression can be arrested and reversed with prompt vascular assessment and treatment.
I think I have Varicose Veins – What should I do?
- See your GP – Your doctor will refer you to have a varicose vein ultrasound and to see a Vascular Surgeon.
- Undergo a Varicose Vein ultrasound - Ideally these are performed at a specialised vascular ultrasound laboratory. We recommend North Shore Vascular Laboratory. The ultrasound scans of your veins (sometimes called a varicose veins doppler or venous insufficiency scan) will help the Vascular Surgeon identify the underlying cause of your varicose veins. With this important information, the Vascular Surgeon can then very quickly start planning what treatment is most appropriate for you. It will also mean they can identify if other scans and/or tests are required.
- Assessment by a Vascular Surgeon – Please bring to your appointment:
- The current referral from your GP, so that you can claim some of the cost of the consultation from Medicare.
- Your varicose vein ultrasounds and/or scans.
- A list of any questions or troubling symptoms you may have.
Your Vascular Surgeon will then discuss your diagnosis and course of treatment with you.
- Treatment
- Non operative
- operative - open surgery or endovenous
The vascular surgeon will take into account the aeitology and anatomy of the venous insufficiency and will advise you on your options of treatment.
- Aftercare - compression
- Wound care - surgery reduces the rate of recurrence of wound
- Recurrence of varicose veins
What if I don’t have my Varicose Veins treated?
If you have a varicose vein that is very small and not causing pain, you may be able to self-manage it with conservative measures, without it worsening.
On the other hand, moderate to severe varicosities can lead to major complications, due to the poor circulation through the affected limb. In this case, prompt treatment can halt and potentially reverse your symptoms.
Left untreated, major complications may include:
- Chronic pain, heaviness, or tenderness.
- Inability to walk or stand for long periods of time.
- Skin conditions /Dermatitis
- Venous Ulcers - skin ulcers especially near the ankle.
- Development of carcinoma or sarcoma (skin cancer) - in long-standing venous ulcers.
- Severe bleeding from minor skin trauma
- Blood Clots - These are frequently isolated to the superficial veins, but can extend into deep veins, becoming a more serious problem.
- Acute Fat Necrosis - especially at the ankle of overweight patients with varicose veins. Females are more frequently affected than males.
If you have developed a varicose vein of any size, it is advisable to explore your treatment options early. Treatment will give you the best chance of reversing any changes that may have taken place in the skin or tissues of the leg.
What treatment options does SVS offer for Varicose Veins?
Sydney Vascular Surgery offers conservative, minimally invasive or surgical treatment options. During your visit, your surgeon will advise you on the best treatment option, or options, available to you. Your surgeon will also perform a general health check that will inform the treatment plan.
Conservative measures include:
- Wearing compression stockings
- Elevating the legs
- Exercising
- Weight optimisation
Minimally Invasive treatments include:
- Sclerotherapy - injecting a solution into the vein to collapse the vein
- Ultrasound-guided foam sclerotherapy - injecting a foam solution into the vein to collapse the vein
Surgical treatments include:
- Vein stripping - removing the affected veins from deep under the surface through a few small incisions.
- Phlebectomy - removing a superficial/surface varicose vein through 2-3 small incisions on the leg.
- VenaSeal - closing off the vein with a medical adhesive, delivered via a catheter.
- Thermal Ablation - destroying the particular veins deep in the thigh and/or the back of the calf that feed the varicose veins using heat, via:
- Endovenous Laser Therapy (EVLT) - guiding a laser fibre inside the vein.
- Radio Frequency (RF) - guiding a heated catheter inside the vein.
Please note: As a general rule, Thermal Ablation will only deal with the underlying cause/source of the varicose veins. These techniques, for most patients, do not remove or destroy the visible varicose veins.
Surgical treatments are given under local and/or general anaesthetic.
Cosmetic Treatment for Varicose Veins
SVS also provides cosmetic treatments for asymptomatic varicose veins. If you have aesthetic concerns or wish to improve the appearance of unsightly varicose veins, book in for an assessment to determine your suitability for treatments such as Sclerotherapy, Thermal Ablation or surgery.
In Summary:
- Varicose veins are twisted and enlarged veins, usually in the legs.
- Varicose vein ultrasound assessment is crucial to determining treatment options.
- Whether they are small or large, diagnosing and treating varicose veins quickly can help to halt and potentially reverse symptoms and complications that may arise.
- Untreated varicose veins can lead to serious complications, such as non-healing skin ulcers, insufficient blood flow, blood clots and chronic leg pain.
- Treatment options range from simple, conservative measures such as compression stockings and exercise, through to surgery.
- Your Vascular Surgeon can best prescribe the most effective treatment plan for you if you bring your varicose vein ultrasound with you to your first appointment.
Helpful Links:
Varicose Veins - http://www.anzsvs.org.au/patient-information/varicose-veins/
Endovenous Therapy – EVLT and RF - http://www.anzsvs.org.au/patient-information/endovenous-therapy-rfa-and-evlt/
Varicose Vein Injections – Sclerotherapy - http://www.anzsvs.org.au/patient-information/varicose-vein-injections-sclerotherapy/
Chronic Venous Insufficiency and Leg Ulcers - http://www.anzsvs.org.au/patient-information/chronic-venous-insufficiency-and-leg-ulcers/







