Chronic / Non-healing Wound Management
 Chronic non-healing wounds are the wounds that do not heal even after a few months or years, secondary to an underlying disease which may interfere with the normal healing process. Chronic wounds can be painful and can adversely affect the quality of life of the patient. Chronic wounds may lead to life threatening complications.
Chronic non-healing wounds are the wounds that do not heal even after a few months or years, secondary to an underlying disease which may interfere with the normal healing process. Chronic wounds can be painful and can adversely affect the quality of life of the patient. Chronic wounds may lead to life threatening complications.
Phases of wound healing
The process of wound healing can be divided into four phases:
Inflammatory phase: This involves a reflex vasoconstriction of the damaged blood vessels, in the wound, which reduces blood loss. Release of inflammatory mediators from the mast cells and damaged tissue causes inflammatory vasodilation which increases the permeability of the adjacent capillaries. Large molecules like fibrinogen escape into the wound area and form long sticky strands of fibrin, providing a framework for clot formation. It also acts as a physical barrier to compartmentalize the wound from the healthy tissue and prevents the spread of infection to the healthy tissue. Vasodilation also leads to localized increase in the flow of blood, increasing the supply of oxygen, nutrients and raw material for the repair of the injury. This occurs within the first 4 hours after the injury.
Destructive phase: Within the next 48 hours’ white blood cells such as neutrophils and macrophages migrate to the wound area, attracted by the mediators released by the damaged tissue and facilitated by the increased permeability of the adjacent capillaries. They clear the dead tissue and any germs in the wound, a process similar to surgical debridement of wounds.
Proliferation phase: Growth factors released from the macrophages and the damaged tissue attracts fibroblasts which synthesize and secrete collagen that aids in repair. This is followed by the formation of new blood vessels (angioneogenesis) and regeneration of epidermis (re-epithelialization). This phase starts about 2 to 3 days after the initial injury.
Remodelling phase: In this phase the scar gradually decreases in size and finally fades away, acquiring the colour of the surrounding skin. This usually starts at about 3 weeks after the injury and may last up to a year or more depending on the size and nature of the wound. This phase involves myofibroblasts.
Factors that delay wound healing
Factors that delay wound healing may include conditions of the immediate wound environment (local factors) as well as conditions affecting the rest of the body (systemic factors). Blood supply to the wound is a crucial factor for wound healing. Thus, wound ischemia or conditions affecting the cardiovascular system can adversely affect wound healing. Immobility reduces the blood circulation and so reduces wound perfusion. Other factors that adversely affect wound healing include infection, presence of foreign body in the wound, poor hygiene, smoking, insufficient diet or malnutrition and psychological stress.
Age also affects wound healing. Wound healing is slower in the elderly, as they have a reduced number of fibroblast in their tissues. This affects the formation of the three-dimensional scaffolding of collagen which is essential for healing. Re-epithelialisation and remodelling phase is also delayed. Moreover, presence of any underlying diseases such as diabetes mellitus, heart disease and peripheral ischemia may further hamper wound healing. Reduced mobility also increases the risk of pressure sore formation.
Common Non-healing wounds
Common non-healing wounds include:
Pressure ulcers: Pressure ulcers are most commonly found over bony areas exposed to excessive pressure such as coccyx or tailbone, buttock, hip and heel. They occur due to reduced blood supply to the area, leading to the death of skin cells and formation of an ulcer. Pressure ulcers are more common in non-ambulatory patients.
Diabetic foot ulcers: Diabetes causes nerve damage that can cause complete loss of sensation in the foot due to which minor foot injuries can lead to ulcers and infections and even gangrene. Diabetic foot is a term used for foot problems in patients with diabetes.
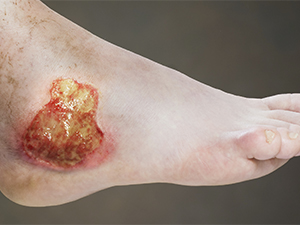
Venous leg ulcers: These ulcers are commonly seen above the ankle. They occur due to insufficiency of the valves in the large leg veins which causes damage to the veins and the blood from the veins oozes out and collects under the skin.
Treatment
Treatment of chronic wounds involves debridement or wound cleaning and wound dressing. Sometimes special therapies such as hyperbaric oxygen therapy, vacuum assisted closure therapy and therapeutic ultrasound may also be used to improve wound healing. Large wounds may sometimes require skin grafts from another part of the body, usually the thigh, to cover them.







